OUR RESULTS
Our PGT-[A]Seq test increases the chance of a healthy birth per embryo transfer
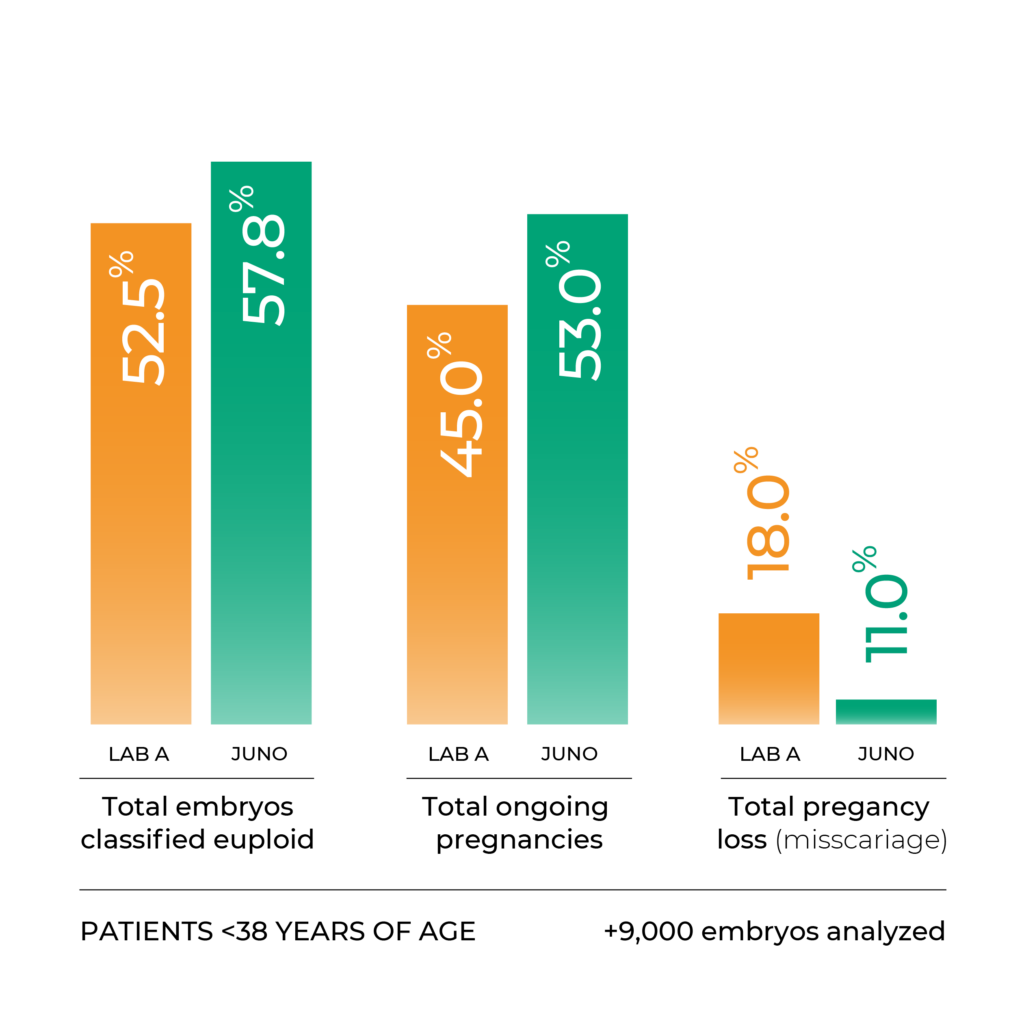

BACKGROUND
An increasing number of IVF cycles include PGT-A to assist in the selection of euploid embryos for transfer to the uterus. All modern PGT laboratories utilise next generation sequencing (NGS) to predict the copy number of each chromosome. Given this technical convergence, it has generally been supposed that the choice of PGT-A provider need only depend on factors such as the quality of the user experience, convenience and price. Here we consider whether the choice of PGT-A provider might have more profound affects, potentially impacting clinical results.

METHODS
A large network of IVF clinics switched from PGT-A provider ‘A’ to provider ‘B’. The final 6 months of clinical data using A was compared to 6 months of data after the switch to B. No significant changes in any aspect of patient population, treatment or embryological practice occurred between the two time periods evaluated.

RESULTS
Within the two time periods considered, 9,091 embryos underwent PGT-A using A and 9,550 using B. The average female age was 39.0 and 39.3, respectively. Differences in important clinical outcomes were observed, which were particularly apparent for female patients <38 years of age. For that group, A versus B results were: 52.5% of embryos classified euploid vs. 57.8% (p<0.0001); 45% ongoing pregnancy after the first embryo transfer vs. 53% (p=0.04); 18% miscarriage rate vs. 11% (p=0.048)..

CONCLUSIONS
PGT-A and NGS are umbrella terms encompassing different methods with widely varying levels of validation and accuracy. The results of this study suggest that the choice of PGT-A provider has implications for clinical results. One possible interpretation of the data is that higher rates of euploidy and pregnancy with B might be a consequence of embryos being wrongly classified as aneuploid by A, while incorrect labelling of abnormal embryos as euploid could explain the relative increase in miscarriage rates when using that provider.